43 year old with Headache and Double Vision-Medical legal implications
- Details
-
Published: Saturday, 15 May 2010 10:53
What are the medical legal implications of the following case?
A 43 year-old man presents to the emergency department (ED) complaining of a severe frontal headache that began suddenly and awakened him from sleep. The headache is associated with nausea, vomiting, and fevers. He also complains of new-onset diplopia (double vision) and photophobia (bright light bothers him), but denies any decrease in visual acuity. He denies experiencing any associated seizures, focal weaknesses, previous similar episodes, frequent headaches, or previous visual disturbances. He does not have any prior significant medical problems, and takes no medication. He drinks socially, does not smoke, and denies recreational drug use.
On physical examination, the patient is ill-appearing but alert and in no apparent distress. His vital signs reveal a temperature of 103.1°F (39.5°C), a blood pressure of 155/95 mm Hg, and a pulse of 110 bpm. The ocular examination demonstrates ptosis of the right eye (droopy eyelid), which is deviated inferolaterally and has a dilated and unreactive pupil. The visual field examination demonstrates bitemporal hemianopsia. Funduscopic examination shows normal venous pulsation and mild bilateral temporal disc pallor. The cranial nerves are otherwise without deficit. The neck is supple and without meningismus. Examination of the chest reveals mild bilateral gynecomastia, without nipple discharge. The lungs are clear to auscultation. Cardiac auscultation reveals a normal S1 and S2 and no murmurs, rubs, or gallops. The abdomen is soft and nontender, and no organomegaly is detected. Bilateral upper and lower extremity strength is 5/5, with normal deep tendon and plantar reflexes. The patient's sensation is intact to light touch and pinprick throughout, and the gait is normal.
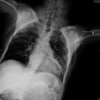
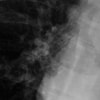
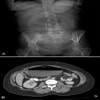
Laboratory investigations reveal a hemoglobin concentration of 13 g/dL (130 g/L); a white blood cell (WBC) count of 16.0 × 103/µL (16.0 × 109/L), with 75% neutrophils; and a platelet count of 340 × 103/µL (340 × 109/L). The electrolyte, blood urea nitrogen (BUN), creatinine, and glucose examinations are all within normal limits. Cerebrospinal fluid (CSF) specimens show 420,000 red blood ceels (RBC)/μL, 20,000 WBC/μL, a normal glucose of 85 mg/dL (4.72 mmol/L), and an elevated protein concentration of 230 mg/dL (2.3 g/L). The CSF Gram stain is negative for bacteria. A computed tomography (CT) scan of the brain is performed, followed immediately by magnetic resonance imaging.
The radiologist misreads the films and the patient is given fever reducing medication and sent home by the emergency physician. He is told to visit his family physician in a few days. The following day, he is found unconscious and is returned to the hospital by ambulance. He is admitted in critical condition and he is re-evaluated. Re-evaluation included a re-examination of his imaging studies by other radiologists.
He is admitted to the ICU undergoes a surgical procedure, but he never regains consciousness, although his vital signs are stabilized. He remained in a vegetative state. The family sued the physicians and the hospital for malpractice.
Discussion
The noncontrast CT scan of the brain when re-reviewed showed a 2-cm sellar mass, with suprasellar extension. There was impingement on the optic chiasm and the hypothalamus, with upward displacement. There was increased density on the right side of the mass, which was suggestive of hemorrhage. The sagittal and coronal T1- and T2-weighted MRI scans demonstrated a large soft-tissue mass in the pituitary fossa, with areas of intermediate- and high-intensity signal suggestive of hemorrhage (see Figure 3). Coronal gadolinium-enhanced T1-weighted images revealed that the mass had a heterogeneous pattern of faint peripheral enhancement (Figure 4). There was evidence of mass effect on the right cavernous sinus, which was most evident in the coronal T1- and T2-weighted images. These findings are consistent with pituitary apoplexy as a result of hemorrhage with or without infarction, likely into a pituitary adenoma. Tests for evaluating the hormonal status of the patient revealed panhypopituitarism. Prior to the acute apoplectic episode, the patient had findings suggestive of central hypogonadism, probably as a component of his hypopituitarism caused by pituitary macroadenoma (diminished libido and bilateral gynecomastia). His neurologic finding (right-sided ptosis with a fixed and dilated pupil pointing downward and outward) was consistent with a right-sided 3rd nerve palsy caused by extension of hemorrhage into the right cavernous sinus.
Pituitary tumor apoplexy is defined as hemorrhage or infarction of a pituitary gland associated with the presence of a preexisting pituitary adenoma. It manifests as a sudden, severe headache, and it is sometimes associated with neurologic and hormonal dysfunction. The word "apoplexy" stems from a Greek term meaning to "have a stroke".[1] Neurologic symptoms and signs are secondary to displacement of the optic nerve and impingement of the 3rd, 4th, and 6th cranial nerves. Hormonal dysfunction results from destruction of the anterior pituitary gland.
Pituitary tumor apoplexy is a rare disorder with an annual incidence of about 1.2 per million.[2] Men are affected twice as often as women, and all age groups can be affected, with the majority of patients in the 5th or 6th decades of life.[3] It is estimated to occur in 1.5-27.7% of cases of pituitary adenoma.[4] Pituitary tumor apoplexy is only rarely associated with a healthy gland; however, approximately 50% of patients who present with pituitary tumor apoplexy are not diagnosed with a pituitary lesion prior to their presentation.[1] All types of pituitary tumors carry the same risk for apoplexy.
The most common symptom of pituitary tumor apoplexy is headache. Almost all patients describe a sudden, severe retro-orbital or bifrontal headache, which is associated with vomiting in two-thirds of cases.[4] The headache and vomiting result from the sudden increase in intrasellar pressure either caused by the hemorrhage or secondary to meningeal irritation from blood or tumor products that leak into the CSF. The increase in intrasellar pressure results in many of the symptoms and signs of pituitary tumor apoplexy.[5] Laterally, the increased pressure causes compression of the structures in the cavernous sinus, namely the 3rd, 4th, and 6th cranial nerves, with the 3rd being most commonly affected as a result of its vulnerable position (parallel to the lateral wall of the pituitary gland). The 6th cranial nerve is the least commonly involved because of its most lateral location within the sinus.
Ophthalmoplegia (caused by 3rd, 4th, and 6th nerve palsies or any combination thereof) is present in around 80% of patients presenting with pituitary tumor apoplexy.[4] Also located within the cavernous sinus is the trigeminal nerve; its involvement may cause facial pain or sensory loss. Carotid siphon compression may present as hemiplegia. Superiorly, the increased pressure compresses the optic chiasm, optic tract, or optic nerve, leading to decreased visual acuity or visual field defects (classically, bitemporal hemianopsia). Blood leaking into the subarachnoid space may result in chemical meningitis with fever, meningismus, and photophobia. Fever in patients with apoplexy may also be explained by alteration in thermal regulation caused by hypothalamic involvement by the hemorrhage or by adrenal insufficiency associated with hypopituitarism. Hemorrhage may extend into the brain parenchyma causing cortical irritation and provoking seizures.
The elevated intrasellar pressure also accounts for the endocrine abnormalities found in cases of pituitary tumor apoplexy. This pressure increase results in compression of the pituitary tissue, compromising its vascular supply and leading to hypopituitarism. Adrenal insufficiency is the most clinically significant result of hypopituitarism, contributing significantly to the mortality of patients with pituitary tumor apoplexy if not promptly recognized and treated. Although not common, patients with pituitary tumor apoplexy may have diabetes insipidus at presentation. The true etiology of diabetes insipidus in this setting is unknown, but it may result from the increased pressure on the pituitary infundibulum, which impedes the antidiuretic hormone from passing from the hypothalamus to the posterior lobe of the pituitary.
A precipitating factor is identified in 50% of cases of pituitary tumor apoplexy. Predisposing factors include dopamine agonist treatment, head trauma, pituitary irradiation, pregnancy, coronary artery bypass grafting, surgical operations, and anticoagulation. Endocrine stimulation tests are also associated with pituitary tumor apoplexy. It is postulated that hormones used in these tests may increase blood flow in pituitary adenomas, provoking bleeding in friable vessels. Pituitary tumor apoplexy following childbirth associated with significant postpartum hemorrhage in nontumorous glands is termed "Sheehan syndrome". The hypertrophy of the pituitary gland that occurs in normal pregnancy combined with the arterial spasm of the pituitary's blood supply (caused by bleeding and hypotension) both contribute to the development of Sheehan syndrome; however the clinical presentation of pituitary apoplexy in these cases is usually less dramatic, with a more gradual development of signs and symptoms of hypopituitarism.
The diagnosis of pituitary tumor apoplexy is best established by MRI; however, this is usually preceded by a rapid diagnostic CT scan to screen for intracranial hemorrhage. MRI is superior to CT scanning for evaluating the pituitary gland and possibly visualizing hemorrhage not seen by CT. In one study, the detection rate of pituitary tumor apoplexy by CT scanning was 21%, whereas the detection rate was 100% with MRI.[3]
Once recognized, effective treatment of pituitary tumor apoplexy requires prompt administration of high-dose corticosteroids. Steroids should be administered in supraphysiologic doses to not only replace endogenous hormone deficiency during a stressful condition, but also to take advantage of its anti-inflammatory effect by decreasing swelling on parasellar structures. The definitive treatment for pituitary tumor apoplexy is emergent surgical decompression. Transsphenoidal resection is the most common approach in this situation. In cases where there is significant extension of hemorrhage into the brain parenchyma beyond the diaphragma sella, an intracranial approach may be preferred. In a minority of cases, conservative medical therapy is an acceptable alternative; examples of this include patients who are poor surgical candidates and selected patients who present with isolated meningismus or ophthalmoplegia and show significant improvement with steroid administration. Medical management includes monitoring of endocrine, neurologic, and ophthalmologic function combined with hormone replacement.
With prompt recognition, timely surgery, and proper medical management, the majority of patients with pituitary tumor apoplexy improve.[6] Ophthalmoplegia is usually the first symptom to resolve. Less readily restored is the optic nerve defect resulting in decreased visual acuity and restricted visual fields. More than half of patients, however, will have permanent hormone deficiencies resulting from pituitary injury and will require hormone replacement. One study showed that maintenance steroid, thyroid hormone, and testosterone replacement was essential postoperatively in 82%, 89%, and 64% of patients, respectively.[7]
Following immediate administration of high dose corticosteroids, the patient in this case underwent an emergent transsphenoidal resection. An infarcted adenoma was identified, with extensive areas of hemorrhage and necrosis consistent with apoplexy. After surgery the swelling in the brain worsened and he remained in a coma. An endocrinology evaluation was completed, and the patient was confirmed to have hypopituitarism, but suffered the effects of significant intracranial bleeding.
The plaintiff's theory of the case was that a correct diagnosis would have resulted in immediate surgery before the patient had bled to a degree where he has lost brain function and consciousness. The jury agreed. The case was taken to court where a plaintiff verdict was returned.
References
- Verrees M, Arafah B, Selman WR. Pituitary tumor apoplexy: characteristics, treatment, and outcomes. Neurosurg Focus. 2004;16:E6.
- Nielsen EH, Lindholm J, Bjerre P, et al. Frequent occurrence of pituitary apoplexy in patients with non-functioning pituitary adenoma. Clin Endocrinol (Oxf). 2006;64:319-22.
- Randeva HS, Schoebel J, Byrne J, Esiri M, Adams CB, Wass JA. Classical pituitary apoplexy: clinical features, management and outcome. Clin Endocrinol (Oxf). 1999;51:181-8.
- Vaphiades MS. Pituitary Apoplexy. eMedicine from WebMD. Last Updated: August 6, 2009. Available at: http://emedicine.medscape.com/article/1198279-overview.
- Zayour DH, Selman WR, Arafah BM. Extreme elevation of intrasellar pressure in patients with pituitary tumor apoplexy: relation to pituitary function. J Clin Endocrinol Metab. 2004;89:5649-54.
- Dubuisson AS, Beckers A, Stevenaert A. Classical pituitary tumour apoplexy: clinical features, management and outcomes in a series of 24 patients. Clin Neurol Neurosurg. 2007;109:63-70.
- Veldhuis JD, Hammond JM. Endocrine function after spontaneous infarction of the human pituitary: report, review, and reappraisal. Endocr Rev. 1980;1:100-7.